Get Complete Project Material File(s) Now! »
aureus and pathogenesis
S. aureus can cause a wide range of diseases, from superficial skin lesions such as abscesses and impetigo to invasive and more serious infections such as endocarditis, osteomyelitis, septic arthritis, and pneumonia (Tong et al., 2015). Some of them are related to a specific production of a single virulence factor, such as enterotoxins in staphylococcal food poising or the TSST-1 in toxic shock syndrome (TSS) (Dinges et al., 2000). However, some of these infections result from multifactorial factors, including septicemia and mastitis in humans and animals, respectively (Dego et al., 2002; Girard and Ely, 2007). In general, every strain of S. aureus can become a life-threatening pathogen depending on host clinical conditions (Wertheim et al., 2005). An important feature of this bacterium is the encoding of some toxins in the core genome or in highly conserved genomic islands, such as α-toxin and phenol-soluble modulins (PSMs), which suggest they are produced by virtually all S. aureus strains (Cheung et al., 2012; Peschel and Otto, 2013).
Colonization and tissue invasion
Adhesion and internalization
The S. aureus pathogenicity is closely related to its capacity to bind directly to the extracellular matrix or host cells mainly mediated by microbial surface component recognizing adhesive matrix molecules (MSCRAMMs) (Heilmann, 2011). The main MSCRAMMs involved in this host cell adhesion is the fibronectin (Fn) binding proteins (FnBPs) that form a bridge with α5β1 integrin on the cellular side (Josse et al., 2017; Sinha et al., 1999). This triggers an intracellular signaling cascade that leads to remodeling of the actin cytoskeleton and internalization of the bacteria (Ridley et al., 2012). High affinity and specificity of FnBPs for Fn are necessary for adhesion and invasion in endothelial cells, although the efficiency of uptake can differ between cell types (Edwards et al., 2010; Josse et al., 2017; Ridley et al., 2012). S. aureus can also adhere and invade non-professional phagocytic cells, such as epithelial, endothelial, fibroblasts, and osteoblasts (Hébert et al., 2000; Josse et al., 2017; Kintarak et al., 2004). In the mastitis context, adhesion and internalization were demonstrated in vitro using bovine mammary epithelial cells (bMEC) (Brouillette et al., 2003; Hébert et al., 2000; Souza et al., 2017). These initial interactions can be affected by the endogenous microbiota, which might express inhibitory properties against pathogens (Woodward et al., 1987). This relation was observed in nasal cavities of healthy hospital staff members in which colonization with corynebacteria was shown to determine low rates of S. aureus (Uehara et al., 2000). This competition was also observed in vitro using lactic acid bacteria isolated from bovine mammary microbiota (Bouchard et al., 2015).
Intracellular survival
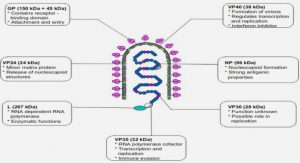
To date, the mechanism by which S. aureus persists in its host is still not fully understood. However, S. aureus has been described as a facultative intracellular pathogen able to survive and persist intracellularly (Fraunholz and Sinha, 2012). In consequence, an intracellular niche might constitute a reservoir for chronic or relapsing staphylococcal infections (Garzoni and Kelley, 2009). S. aureus can interact with integrins and adhere in non-phagocytic cells such as the bovine mammary epithelial cells (bMEC) of the MG with subsequent internalization (Figure 6), which corresponds to an important mechanism of evasion from host immune responses (Bouchard et al., 2013; Sibbald et al., 2006).
Figure 6. Pathogenic mechanisms that offer some advantages to the spread and survival of S. aureus. S. aureus cell wall-anchored (CWA) proteins are associated with interaction and recognition by host cells, which enable the adhesion to the extracellular matrix and consequent biofilm formation. When recognized by host receptors, S. aureus may stimulate the production of cytokines and pro-inflammatory chemokines. S. aureus can be internalized by the host cells, causing cell apoptosis, or can remain dormant in a state known as small colony variants (adapted from Foster et al., 2014).
Small-colony variants (SCVs)
SCVs are a subpopulation of S. aureus with a phenotype characterized by small size colonies, slow growth rate and particular biochemical and morphological properties. S. aureus persistent and relapsing infections are mainly associated with this phenotype. It enables to “hide” inside host cells without causing significant damage and confers resistance against host immune responses and antimicrobial therapy (Gordon and Lowy, 2008; Sendi and Proctor, 2009). When back in favorable conditions, S. aureus can revert to the virulent wild-type phenotype, which possibly results in recurrent infections (Proctor et al., 2006). Beside chronic mastitis, S. aureus SCVs formation was also associated with intracellular persistence in rhinosinusitis and osteomyelitis (von Eiff et al., 1997; Tan et al., 2014).
Biofilms
When bacteria adhere to a surface, they grow and form complex communities referred to as biofilms (Figure 6). Bacterial biofilms consist of packed bacteria within extracellular polymeric substances (EPS) containing polysaccharides, extracellular DNA, and proteins that are difficult to penetrate and disrupt (Manning and Kuehn, 2013). This organization confers selective advantages for the bacteria under environmental conditions (e.g. resistance to antimicrobial agents and to desiccation) (Costerton et al., 1999). Interestingly, most of the mastitis-associated strains have the capacity to organize and form biofilm, which can suggest a correlation with the high recurrence of this infection in the udder (Szweda et al., 2012). In the nosocomial environment, biofilm-associated S. aureus induce infections, such as intravascular catheter-related sepsis and infective endocarditis, that lead to high morbidity (Archer et al., 2011; Silva-Santana et al., 2016).
Antimicrobial resistance
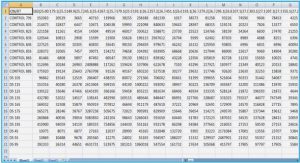
S. aureus is the best opportunistic pathogen to exemplify the adaptive evolution of bacteria in the antibiotic era (Table 2). Its broad resistance to practically all of the early antibiotic classes is mediated almost exclusively by determinants acquired via horizontal DNA transfer. The scarcity of effective treatment against S. aureus led to high mortality in hospitals until the introduction of penicillin in the 1940s (Chain et al., 1940). The antimicrobial agent penicillin binds to staphylococcal penicillin-binding proteins (PBP), resulting in the inactivation of an essential transpeptidase which inhibits bacterial cell wall synthesis. S. aureus resistance is due to the production of an enzyme called beta-lactamase that hydrolyzes the amide bond of the beta-lactam ring, resulting in functional loss of the antibiotic. The production of this enzyme is encoded by the structural gene blaZ (Pantosti et al., 2007). However, as early as 1942, the first case of penicillin-resistant staphylococci was described (Table 2) (Rammelkamp and Maxon, 1942). Methicillin (semisynthetic β-lactam) was then introduced in 1961 and it was rapidly followed by cases of methicillin-resistant isolates (MRSA) (Jevons, 1961). Methicillin resistance is due to the expression of an additional penicillin-binding protein (PBP2a), with reduced affinity for beta-lactams. This protein is a product of the mecA or mecC genes carried in a staphylococcal chromosomal cassette mec (SCCmec) element (Kaya et al., 2018; Pantosti et al., 2007). Genetic rearrangements of SCCmec element can result in variant elements, indicated by Roman numerals SCCmec types (I to XIII) (Baig et al., 2018). Initially described in a British hospital, Hospital-acquired (HA-MRSA) isolates quickly reached a global scale (Lowy, 2003) and subsequently being recognized in the communities (CA-MRSA) (Chambers, 2001). The emergence of CA-MRSA infections in healthy individuals suggested an increase in the S. aureus pathogenicity (Liu, 2009). In addition, CA-MRSA carries smaller SCCmec types and spread more easily when compared to HA-MRSA (Aires-de-Sousa, 2017).
Vancomycin was then introduced in the treatment of infections caused by methicillin-resistant bacteria (Levine, 2006). In 1997, the first report of vancomycin intermediate-resistant S. aureus (VISA) came from Japan (Hiramatsu et al., 1997), with reduced susceptibility as result from changes in bacterial peptidoglycan biosynthesis. However, full resistance to this antibiotic (VRSA) was further reported from strains that acquired by conjugation the vanA operon from vancomycin-resistant Enterococcus faecalis (Ahmad, 2018; Lowy, 2003).
aureus isolates from mastitis
Comparative analysis between genomes of different S. aureus strains allowed to observe host-specific genotypes that emerged after a host jump between human and animal hosts (Guinane et al., 2010). This passage then led to an adaptive evolution with a genomic heterogeneity between strains. However, S. aureus populations are clonal and isolates belonging to the same lineage are strongly conserved, even when separated by time and space (Lindsay, 2014).
Typing technique using molecular biology, like Multi Locus Sequence Typing (MLST), enables determining the sequence types (ST) of each strain, that are grouped into clonal complexes by their similarity to a central genotype (Smyth et al., 2009). The majority of ruminants isolates from mastitis are represented by few clonal complexes, including CC97, CC705 (ST151), CC130, and CC126 in cows and CC133 in small ruminants (sheep and goat) (Figure 7) (Fitzgerald, 2012; Guinane et al., 2010). Furthermore, isolates of the CC133 can also be occasionally associated with IMI in cows (Smyth et al., 2009); however, some subtypes, as ST151, were exclusively associated with bovine mastitis and have not been detected among humans (Fitzgerald, 2012; Guinane et al., 2010; Sakwinska et al., 2011), suggesting some kind of specialization in terms of host. For instance, bovine-adapted genotype belonging to CC8 were reported in Switzerland and was described as the result of a host shift from humans to cows with loss of genes necessary for human carriage (Sakwinska et al., 2011).
Table of contents :
Chapter 1. Literature review
3.1. Mastitis
3.1.1. General considerations
3.1.2. S. aureus mastitis
3.1.3. Mammary gland defenses
3.1.3.1. Anatomic and microbial barrier
3.1.3.2. Innate immune response
3.1.3.3. Adaptive immune response
3.1.4. Diagnosis
3.1.5. Control
3.1.5.1. Prevention
3.1.5.2. Treatment
3.2. Staphylococcus aureus
3.2.1. Staphylococcus spp.
3.2.2. Staphylococcus aureus
3.2.3. Biology of S. aureus
3.2.3.1. Molecular determinants of virulence and pathogenicity
3.2.3.2. Virulence regulation systems
3.2.3.3. Virulence factors
3.2.4. S. aureus and pathogenesis
3.2.4.1. Colonization and tissue invasion
3.2.5. S. aureus isolates from mastitis
3.2.5.1. Virulence factors associated with ruminant mastitis
3.3. Extracellular vesicles
3.3.1. Overview of extracellular vesicles
3.3.1.1. Eukaryotic EVs
3.3.1.2. Bacterial EVs
3.3.2. Biological roles of bacterial EVs
3.3.2.1. Bacteria-host interactions
3.3.2.2. Elimination of harmful material
3.3.2.3. Biofilm formation
3.3.2.4. Nucleic acid and horizontal gene transfer
3.3.2.5. Interactions within bacterial communities
3.3.2.6. Threat avoidance
3.3.2.7. Adaptation to environmental conditions or variations
3.3.3. Biogenesis of bacterial EVs
3.3.3.1. Genetic factors associated to EVs release
3.3.4. EVs in Gram-positive bacteria
3.3.4.1. S. aureus EVs
3.3.4.2. EVs in other Gram-positive pathogenic bacteria
3.3.4.3. Non-pathogenic bacterial EVs
3.3.5. Vaccines and applications
3.4. Extracellular vesicle isolation and characterization techniques
3.4.1. Isolation methods
3.4.2. Current methods for EVs analysis
4. Context and aim of the Ph.D. project
4.1. Context of the thesis project
4.2. Aim of the Ph.D. project
5. Chapter 2. Immunomodulatory effects induced by S. aureus extracellular vesicles 87
6. Chapter 3. Comparative proteomics of EVs released by human, bovine and ovine S. aureus strains
7. Chapter 4. Critical analysis and perspectives
7.1. General discussion and conclusions