Get Complete Project Material File(s) Now! »
Bartonella interaction with endothelial cells
Another remarkable pathologic feature of Bartonella infection is that it causes vasoproliferative lesions in a process of pathological angiogenesis (Dehio, 2004). Typical manifestations of Bartonella-triggered tumor formation are verruga peruana (B. bacilliformis) and bacilliary angiomatosis (BA) (B. quintana and B. henselae). The lesions consist of proliferating endothelial cells, bacteria and a mixture of macrophages/monocytes and polymorphonuclear neutrophils (Kostianovsky and Greco, 1994; Manders, 1996). Bartonella were found in aggregates both surrounding and within endothelial cells. Clearance of the infection by antibiotics caused complete regression of vascular lesions, indicating that vascular endothelial cells are a target for Bartonella colonization in vivo (Manders, 1996). Primary human umbilical vein endothelial cells (HUVEC) have been used as a model to study the interaction between the human vascular endothelium and Bartonella. Infection of vascular endothelial cells with Bartonella in vitro results in cytoskeletal rearrangements that mediate bacterial internalization caused by activation of the small GTPase Rho (Dehio, 2001); activation of transcription factor nuclear factor NF-kappaB, which mediates recruitment and adhesion of leukocytes (Fuhrmann et al., 2001); inhibition of apoptosis (Kirby and Nekorchuk, 2002); and direct mitogenic stimulation (Conley et al., 1994), resulting in endothelial proliferation and formation of vasoproliferative tumors (Pulliainen and Dehio, 2009). These cellular changes might be linked to Bartonella trimeric autotransporter adhesins (TAAs) (BadA) (see below) (Riess et al., 2004) and the VirB/VirD4 type IV system (Schulein et al., 2005).
BadA
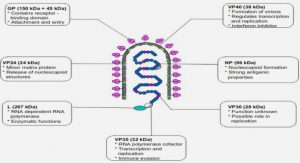
Bartonella adhesion A (BadA) of B. henselae (Riess et al., 2004), together with variably expressed omps (Vomps) of B. quintana (Zhang et al., 2004) and Bartonella repetitive protein A (BrpA) of B. vinsonii (Zhang et al., 2004), are defined as Bartonella trimeric autotransporter adhesins (TAAs). TAAs are widespread in α-, β-and γ-proteobacteria and are related to the pathogenicity of many Gram-negative bacteria (Girard and Mourez, 2006). All share a similar trimeric ‘lollipop-like’ structure. They have been designated as membrane anchor, stalk, neck and head, respectively (Linke et al., 2006) (Fig 6).
T4SS: the VirB/VirD4 type IV system
As described above, the VirB/VirD4 type IV system was shown to be related to endothelial cell parasitism. In fact, the VirB/VirD4 type IV system was revealed to be a 17 kDa immunodominant antigen, a VirB5 homolog encoded in the virB operon in B. henselae (Padmalayam et al., 2000). Subsequently, the VirB/VirD4 type IV system was widely studied. The VirB/VirD4 type IV system of B. henselae is able to transport Bartonella effector proteins (Beps) BepA to BepG, which are encoded downstream from the virB/virD4 locus of B. henselae (Schulein et al., 2005), into the host cell cytosol (Schmid et al., 2006). These Beps contain a conserved Bep intracellular delivery (BID) domain close to the C-terminus, which, together with a C-terminal positively charged tail sequence, constitutes a bipartite signal for T4SS-mediated protein translocation (Schroder et al., 2011). The main functions of the Beps are as follows: modification of the endothelial cell, including formation of the cellular structure invasome that mediates cell invasion (Rhomberg et al., 2009); activation of proinflammatory reaction factors (nuclear factor (NF)-κB, IL-8, ICAM-1); inhibition of endothelial cell apoptosis; and capillary-like sprout formation of endothelial cell aggregates (O’Rourke et al., 2011). The functions of BepA to BepG have recently been studied. BepA inhibits endothelial cell apoptosis and is responsible for capillary sprout formation in a more complex infection model (Schmid et al., 2006). BepF has been implicated in triggering the formation of invasomes together with BepC (Truttmann et al., 2011). BepG, that triggers cytoskeletal rearrangements, potently inhibits sprout formation (Scheidegger et al., 2009). Recently, it has been demonstrated that the virB/virD4 system of B. henselae is able to transfer DNA into endothelial cells, and BepD increases the transfer rate, suggesting that T4SS-dependent DNA transfer into host cells may occur naturally during human infection with Bartonella, and its capacity for DNA transfer increases its potential use in gene therapy and vaccination (Schroder et al., 2011).
Bartonellae and their vectors
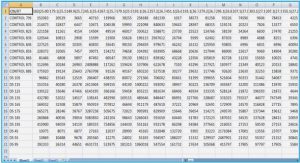
Bartonella species are transmitted to mammals by various arthropod vectors, mainly including sandflies (Townsend, 1913), human lice (Varela et al., 1954), cat fleas (Chomel et al., 1996), some rodent fleas (Morick et al., 2010), various hard tick species (Eskow et al., 2001; Kruszewska and Tylewska-Wierzbanowska, 1996) and various biting fly species (Dehio et al., 2004; Halos et al., 2004). A single mammal host may be infected by many Bartonella species (Table 1) and one vector can also be infected by various Bartonella species (Bown et al., 2004; Rolain et al., 2003b). However, the diversity of Bartonella species DNA identified in ectoparasites is much broader than that of species detected in their mammalian hosts (Tsai et al., 2011a; Tsai et al., 2011b), suggesting that Bartonella species are better adapted to their vectors than to their mammal hosts (Tsai et al., 2011a). Mechanisms leading to fitness in vectors and their mammal hosts warrant further experimental investigation.
bacilliformis and sandflies
Lutzomyia verrucarum, a native sandfly species in Peru, is the natural vector of B. bacilliformis (Townsend, 1913). Townsend was the first to propose L. verrucarum as an etiological agent of human bartonellosis (Oroya fever) based on epidemiological data (Townsend, 1913). Subsequently, in order to experimentally demonstrate that B. bacilliformis is the etiological agent of human bartonellosis, several experimental infection models were created in monkeys, which are able to reproduce B. bacilliformis bacteremia (Noguchi et al., 1929). Battistini et al., (1931) established that sandfly bites can induce verruga peruana in monkeys under experimental conditions; they demonstrated that B. bacilliformis could be isolated from blood of infected monkeys, and they revealed the presence of B. bacilliformis in midgut and feces of sandflies (Battistini, 1931). In addition to L. verrucarum, another unknown vector might exist as a potential transmission vector because of inconsistency between the distribution of Carrion’s disease and L. verrucarum (Scheidegger et al., 2009).
quintana and human body lice
The ability of body lice (Pediculus humanus corporis) to transmit B. quintana was first reported in 1920 (Byam and Lloyd, 1920). Recently, B. quintana was detected by PCR in body lice of homeless persons in France, Russia, Japan and the USA (Bonilla et al., 2009; Foucault et al., 2002; Rydkina et al., 1999; Sasaki et al., 2002). B. quintana replicates in the louse intestinal tract without affecting the life span of the louse (Seki et al., 2007). Transmission to humans is thought to be due to inoculation during scratching of B. quintana contained in louse feces. (Raoult and Roux, 1999). B. quintana is able to survive and remain infectious up to one year in louse feces (Kostrzewski, 1950). Up until now, there has been no evidence demonstrating that B. quintana can be transmitted to offspring (eggs and larvae) of infected lice. In addition to humans, B. quintana is also able to infect other mammals (monkeys, cats and dogs) (Breitschwerdt et al., 2007; Kelly et al., 2006; O’Rourke et al., 2005). B. quintana can also be detected in cat fleas (Rolain et al., 2003b) and ticks (Chang et al., 2001).
henselae and cat fleas
The role of cat fleas (Ctenocephalides felis) in transmission of B. henselae was reported in northern California in the early 1990s (Koehler et al., 1994). Subsequently, it was experimentally demonstrated that infected fleas can transmit B. henselae to cats (Chomel et al., 1996). B. henselae replicates in the gut of the cat flea and is able to survive several days in flea feces (Chomel et al., 2009). Bacteria were shown to be present in flea gut 3 h post-feeding, and persisted for more than 9 days after inoculation (Higgins et al., 1996). Similarly to louse feces, flea feces appear to be the principal infectious source of B. henselae. Transmission from cats to humans occurs through cat scratch. Apart from cat scratch, the role of cat bites in transmission has also been suggested (Demers et al., 1995; Jendro et al., 1998).
Transferrin and lactoferrin iron transport
Many bacterial species such as Neisseria and Haemophilus influenzae have transferrin and/or lactoferrin receptors (Cornelissen and Sparling, 1994; Fuller et al., 1998). Iron is stripped by these receptors from transferrin and lactoferrin and iron-free proteins are released. The functional transferrin receptor in Neisseria consists of TbpA and TbpB subunits. TbpA is analogous to TonB-dependent outer membrane receptors and TbpB is a lipoprotein anchored in the outer leaflet of the outer membrane (Legrain et al., 1993). TbpA is strictly required, whereas the requirement for TbpB is not as stringent. Uptake of iron by TbpA is TonB-ExbB-ExbD and pmf-dependent (Cornelissen et al., 1997). The bipartite lactoferrin LbpAB receptors of Neisseria (Schryvers et al., 1998) and H. influenzae (Ekins et al., 2004) function similarly, with only Fe(III) crossing the outer membrane. In the periplasm, Fe(III) binds FbpA in association with the bipartite receptor TbpAB (Gomez et al., 1998). FbpA shuttles Fe(III) across the periplasm to an ABC permease in the cytoplasmic membrane (Ekins et al., 2004). This ABC permease translocates ferric iron across the cytoplasmic membrane into the cytosol.
Synthesis and excretion of siderophores
To overcome the problem of the low solubility of Fe (III), many bacteria synthesize and secrete strong iron chelators: siderophores. Siderophores chelate iron from the extracellular medium; the iron-loaded siderophore is then taken up by the cell through a specific uptake system (Fig.2). Siderophores are low-molecular-weight compounds (400 to 1,000 Da) produced by microorganisms. They are synthesized by non-ribosomal cytoplasmic peptide synthetases resembling machinery used for the biosynthesis of peptide antibiotics. Following their synthesis, siderophores are excreted into the extracellular medium. These molecules are thought to be too large to diffuse through the envelope. In E. coli, entS, which is located in the enterobactin biosynthesis and transport gene cluster, encodes a membrane protein belonging to the major facilitator superfamily. The proteins of this family are involved in proton motive-force-dependent membrane efflux pumps. The protein EntS was shown to be directly involved in enterobactin export (Furrer et al., 2002).
Table of contents :
Chapter one Bartonella and its survival in different microenvironments
1. Analysis of Bartonellae genomes
2. Diseases caused in humans; diagnosis and treatment of Bartonellosis
3. The cycle of Bartonella in the mammalian reservoir host
4. Bartonella and erythrocyte parasitism
5. Bartonella interaction with endothelial cells
6. Bartonellae and their vectors
Chapter two Iron/Heme uptake in Bartonella
1. Free Fe(II) and its transport
2. Transferrin and lactoferrin iron transport
3. Siderophore and Hemophore
4. Receptors for siderophores and heme/hemophore
5. The TonB-ExbB-ExbD complex
6. Transport across the periplasm and cytoplasmic membrane
7. Fate of the ferri-siderophore and heme in the cytoplasm
8. Regulation of iron and heme uptake in Gram-negative bacteria
9. The heme uptake system in Bartonella
Chapter three Research significance and Purpose of the work
Results
Paper one Heme degrading protein HemS is involved in oxidative stress response of Bartonella henselae
State of the art concerning the fate of heme in the cytoplasm
Paper two Heme binding proteins of Bartonella henselae are required when undergoing oxidative stress during cell and flea invasion
State of the art concerning outer membrane heme binding proteins of Bartonella
1. Outer membrane heme binding proteins in Gram-negative bacteria
2. The finding of heme binding proteins in Bartonella and their structure
3. Heme binding proteins cannot transport heme
4. Heme binding proteins and interactions with the infected host
5. Regulation of expression of heme binding proteins in Bartonella
Discussion Discussion and perspectives
Supplement Paper Identification of a novel nanoRNase in Bartonella
References References