Get Complete Project Material File(s) Now! »
CHAPTER II LITERATURE OVERVIEW OF CANCER AND BREAST CANCER
CANCER AND BREAST CANCER STATISTICS
Introduction
Breast cancer is the most prevalent cancer for women of all ages throughout the world and ranks as the second highest cause of death. Breast cancer is a major health risk for all women with global statistics showing that the annual occurrence of the disease is escalating (Brem & Kumar, 2011; Howlader, Chen, Ries, Loch, 2014; Reyes-Gibby et al., 2012; Travado & Reis, 2013; Vahdaninia, Omidvari & Montazeri, 2010; Wong & Bloom, 2005). According to the National Cancer Registry network, one in every twenty-six South African women will be diagnosed with breast cancer with approximately 5% younger than 35 years of age. This makes breast cancer the number one malignancy amid women in South Africa (Van Oers & Schlebusch, 2013).
Early and progressed cancer screening and advances in clinical oncology have noticeably led to protracted survival rates in breast cancer patients with percentages as high as 95 when discovered early enough (Cielito et al. 2012; Hummel et al., 2015; Vorobiof, Sitas & Vorobiof, 2001; Weis, Poppelreuter & Bartsch, 2009). According to Fiszer and colleagues (2014) survival after 5 years for early localized breast cancer is now above 96%, while 82% of all women diagnosed with breast cancer can anticipate surviving 10 years.
Survivors of breast cancer are officially the leading group of cancer survivors amongst women in the Western world (Fiszer, Dolbeault, Sultan & Bredart, 2014). For this reason we see the added interest and research on health related quality of life and the critical need to find creative strategies to assist this population in coming to terms with the cancer reality (Greeff, 2008; Hummel et al., 2015).
Cancer as a chronic illness
The progress and advances in the oncology discipline over the last 15 years have led to the reality that cancer is no longer seen as a death sentence since people with cancer are living longer (Greeff, 2008; McCorkle, Ercolano & Lazenby, 2011; Naus, Ishler, Parrot & Kovacs, 2009). Cancer as a chronic illness not only challenges old school theories that an oncologist’s work is completed after treatment, but also requires of patients to acknowledge their cancer as a chronic illness with accepting their own participation in the management of their illness (McCorkie et al., 2011). Cancer care, as a chronic illness, occurs on a scale that extends from early detection and diagnosis to the end of life, with treatment, side-effects and survivorship in between (McCorkle et al., 2011).
Definition of chronic illness
Chronic illness or disease can be defined as a long-lasting condition or illness that can be restricted or controlled but not cured and which affects the population worldwide (Arbor, 2011). In the last decades, there have been dramatic shifts in the precedent of diseases from infectious diseases to the present leading causes of mortality dominated by chronic illness. There has been an explosive rise in the incidence of chronic illness in recent years, especially coronary heart disease, diabetes and cancer. These chronic illnesses are viewed as the most common, costly and deadly medical conditions to society and will impose a large liability in the future (Barsky, Friedman & Rosen, 2006; Fortin, Chouinard, Bouhali, Dubois, Gagnon, & Bélanger, 2013; Wright & Kirby, 1999). According to Naus and colleagues (2009) the Census Bureau has projected that over the span of the next 50 years the number of cancer survivors will escalate at a bigger ratio than the occurrence of cancer itself. This estimation proposes the importance of creating a clearly defined model of cancer as a chronic illness in relations to medical treatments and quality of life outcomes.
Chronic illness and emotional and sexual outcomes
Most chronic illnesses like diabetes mellitus, cardiovascular disease and cancer, with their associated treatments, carry a high risk for emotional distress and sexual dysfunctions (Carpenter, Andersen, Fowler, & Maxwell, 2009; Nusbaum, Hamilton & Lenahan, 2003; Richards, Bertolotti, Doss & McCullagh, 2011). A chronic illness can disturb the quality of life of a person through its antagonistic consequences on, amongst other things, sexual functioning which are often long-term and permanent (Barsky et al., 2006). The emotional impression of an initial cancer diagnosis, its consequent treatment and chronicity can have an extreme and overpowering influence on the patients’ quality of life (Nekolaichuk et al., 2012). This will be discussed at length later in this chapter.
Different types of cancer with their emotional and sexual side-effects
A study done by Nekolaichuk and colleagues (2012) have shown that in recent years survival for all types of cancers has grown noticeably from 56% to 62% resulting in patients living longer with prolonged sequelae. According to Katz (2005) and Carpenter and co-workers (2009) the diagnosis of any form of cancer has a distressing impact on the psychological, emotional and sexual welfare of the patient.
The group of cancers (gynaecologic cancers, prostate- and testicular cancers) that are under discussion here are very similar to breast cancer in symptoms, treatments and side-effects, as well as the influence on the patient’s quality of life. There are also very clear resemblances between these cancers and breast cancer in terms of the lack of existing research concerning specific guidelines and open communication between patient and treating practitioner that are adequate to address the sexual and emotional demands of this specific cancer population.
Gynaecologic cancers
Endometrial-, ovarian- and cervix cancer, are the three most common gynaecologic cancers. Gynaecologic cancer patients, especially survivors of ovarian cancer have been found to be a high risk for developing depression, anxiety and chronic sexual dysfunction. With the cumulative number of patients attaining long term survival following early stage cervical and endometrial cancer, emanates the need to expand existing understanding of post-treatment sexual adjustment and rehabilitation requirements of this specific population (Juraskova, Butow, Bonner, Robertson, & Sharpe, 2013).
Gynaecologic cancer patients, much like prostate cancer patients, undergo early declines in sexual activity and disturbed responsiveness that can end in a permanent sexual dysfunction (Carpenter et al., 2009). Cervix and endometrial cancers can be treated with radical or total abdominal hysterectomy as part of the surgical treatment plan, which result in the removal or alteration of the sex organs that anatomically influences the cancer patients’ sexual functioning (American Cancer Society, 2013; Seungtaek & Eifel, 2009). Because of curative treatments, 85% to 90% of patients with stage 1 cervical cancer will survive their cancer ordeal, needing interventions from the oncology team that can improve their quality of life (Phaendler, Wenzel, Mechanic, & Penner, 2015).
A study done by Phaendler, Wenzel, Mechanic and Penner (2015) shown that cervical cancer patients have worse quality of life scores, not only when compared with the overall population, but also with other gynaecologic cancer patients and survivors. These authors noted that patients with invasive cervical cancer who undergo radical surgery and radiation therapy, scored lower in physical, psychological and sexual domains which ultimately disrupt long-term quality of life. Psycho-social problems affecting quality of life in cervical cancer survivors include mood and stress disorders, body image, and fear of recurrence. In the intense setting among cervical cancer patients treated with high-dose rate brachytherapy, 30% experience acute stress disorder (intrusive memories, vegetative hyper arousal, and avoidance reaction) one week after the end of their treatment (Fossa, Dahl, 2006). The sexual impact is maybe more prominent amongst cervical cancer survivors because of the younger age (average of 50 years) at the onset of cervical cancer. It is essential to keep finding ways to open the door for survivors to continue to talk about their experience, as is necessary for their sense of continued healing and social support, whether that be with family, friends, or health care providers (Fossa & Dahl, 2006).
Prostate cancer
According to McCaughan and colleagues (2013) and the American Cancer Society (2010) prostate cancer accounts for approximately a quarter of all new male cancer diagnoses each year in the UK and North America. In all South Africa population groups, prostate cancer was also the most common male cancer excluding basal cell carcinoma (Babb, Urban, Kielkowski, & Kellett, 2014). Patients with clinically localized prostate cancer have a positive long-term overall and cancer-specific degree of survival regardless of treatment choice (Koyama, Kang-Hsien, Albertsen, et al., 2013).
Since the median life expectancy after treatment for prostate cancer is 13.8 years, a thorough assessment of long-term functional outcomes (very much the same as in breast cancer) is vital to an understanding of the complete experience of men living with a diagnosis of prostate cancer. According to Resnick and colleagues (2013), literature only reports outcomes in terms of health-related quality of life in patients with prostate cancer that are short-term (1-3 years) or intermediate-term (4-5 years), which might not indicate the long term experience of prostate cancer patients. Prostate cancer patients who undergo a prostatectomy (a surgical operation to remove all or part of the prostate gland) were five times more prone to have urinary incontinence and twice as likely to have erectile dysfunction as the patients who went through radiotherapy. Men in the prostatectomy group were considerably more prone than those in the radiotherapy group to report having erections insufficient for intercourse at two and five years post treatment. Sometimes the erectile dysfunction also goes with urinary incontinence (Resnick et al., 2013).
CHAPTER I: INTRODUCTION
1.1 OVERVIEW AND STATISTICS
1.2 BREAST CANCER AS THE MAIN SUBJECT OF THIS STUDY
1.3 PHASES OF BREAST CANCER
1.4 THE DIFFERENCE BETWEEN THE TERM BREAST CANCER PATIENT AND BREAST CANCER SURVIVOR
1.5 THE CHRONICITY OF BREAST CANCER SURVIVORSHIP
1.6 BREAST CANCER AS A TRAUMATIC EVENT
1.7 BREAST CANCER AND PSYCHOLOGICAL DISTRESS
1.8 BREAST CANCER AND SEXUAL FUNCTIONING
1.9 PSYCHO-ONCOLOGY
1.10 PSYHO-ONCOLOGIC INTERVENTIONS
1.11 AIMS AND RATIONALE OF THIS STUDY
1.12 METHODOLOGY
1.13 OVERVIEW OF THE THESIS
CHAPTER II LITERATURE OVERVIEW OF CANCER AND BREAST CANCER
2.1 CANCER AND BREAST CANCER STATISTICS
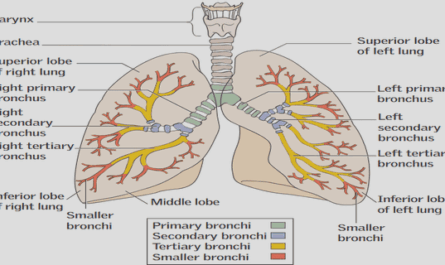
2.2. THE BIOLOGY OF BREAST CANCER
CHAPTER III PSYCHO-ONCOLOGY– A THEORETIC OVERVIEW
3.1 INTRODUCTION
3.2 THE BIO-MEDICAL MODEL
3.3 THE BIO-PSYCHO-SOCIAL MODEL
3.4 PSYCHO-ONCOLOGY
CHAPTER IV PSYCHO-ONCOLOGIC INTERVENTIONS FOR THE BREAST CANCER PATIENT
4.1 INTRODUCTION
4.2 AIMS AND BENEFITS OF CANCER-RELATED THERAPEUTIC INTERVENTIONS
4.3 INDIVIDUAL PSYCHOTHERAPY AND CANCER-RELATED INTERVENTIONS
4.4 THERAPEUTIC INTERVENTIONS FOR BREAST CANCER PATIENTS
CHAPTER V SEX THERAPY AS A PSYCHO-ONCOLOGIC INTERVENTION FOR BREAST CANCER PATIENTS .
5.1 INTRODUCTION
5.2 DEFINITION AND DESCRIPTION OF SEX THERAPY
5.3 AIMS AND BENEFITS OF SEX THERAPY
5.4 SPECIFIC INTERVENTIONS IN SEX THERAPY PRACTICE
5.6 PRACTICAL IMPLICATIONS AND SUMMARY
CHAPTER VI RESEARCH METHOD: CASE STUDY DESIGN
6.1 AIMS OF THE STUDY
6.2 PHILOSOPHICAL, PARADIGM AND INTERPRETIVE FRAMEWORKS AND DEFINITIONS
6.3 QUALITATIVE RESEARCH
6.4 SUMMARY
CHAPTER VII FINDINGS
7.1 INTRODUCTION
7.2 PARTICIPANT DESCRIPTION
7.3 CATEGORIES AND THEMES: THE VOICES OF THE PARTICIPANTS 272
7.4 CATEGORIES AND THEMES: INDIVIDUAL PSYCHO-ONCOLOGIC INTERVENTIONS
7.6 SUMMARY
CHAPTER VIII Discussion and Conclusions
8.1 DISCUSSION
REFERENCES
GET THE COMPLETE PROJECT