Get Complete Project Material File(s) Now! »
CHAPTER FOUR INITIATING STUDENTS INTO THE CULTURE OF THERAPEUTIC PSYCHOLOGY
The way in which psychological treatment is presented in novels (Green, 1964; Kesey, 1962; Rosten, 1961; Schreiber, 1973), movies, even text books and classrooms, is not the same as in practice. In real live situations, the events that occur in psychotherapy, and the really decisive moments that take place, as every patient or therapist who has experienced them knows, “…are unpredictable, unique, unforgettable, always unrepeatable, and often indescribable” (Laing, 1974, p. 47). During the Medunsa selection process, students from many South African Universities with different theoretical backgrounds, apply to do the MSc Clinical Psychology course. During their internship year many students remark that they find it difficult to translate their theoretical knowledge into practice. A frequent remark made by the interns, is that role-playing is vastly different from interacting with a real patient in a real psychotherapeutic setting. Unlike the broad theoretical contents relating to psychotherapy as expounded in the previous chapter, in the present chapter and in Chapters 5 to 8, I will outline eight specific theoretical approaches of which I typically share with intern-psychologists during their internship training and supervision at the hospital. My personal attitudes about each theoretical approach at the beginning of each section are meant to encourage dialogue with interns. Because interns have been required to demonstrate their knowledge in ecosystemic psychotherapy in their written and oral examinations, I encourage them to keep an open mind during their internship year, by acquiring knowledge and practical skills belonging to all eight theoretical approaches.
Theoretical Perspectives in Psychotherapy
In this chapter the challenge will be, to connect the natural everyday group sharing activities in the hospital, to the theoretical issues of psychological treatment and training?
The challenge then is how to move from my personal experiences and observations, to the general theories and models of treatment and training. In doing so I will endeavour to reconcile the tension between the realities of what happens in the hospital, and the ideal as presented in the theoretical models used. By remaining rooted in the reality experiences of the hospital, I propose to relate to the eight theoretical approaches used, and show how the main aspects of the theoretical models have been effective in the practical application thereof.
Relating and linking the experiences outlined in this and the following chapters, to theories of psychotherapy, and taking cues from how psychotherapy has evolved over the past 120 years, (Bergin & Garfield, 1994; Freedheim, 1992, 2003; Lambert, 2004; Zeig, 1987, 1992, 1997), and the many multicultural aspects of psychotherapy (Corey, 2000, 2001, 2005; Moodley & Palmer, 2006; Multicultural Psychotherapy Associates, 2004, 2006; Prochaska & Norcross, 2007), the following eight broad therapeutic models will be referred to. Also, keeping in mind Bergin and Garfield’s (1994) reminder to clinicians that, “…no single profession has a monopoly on the field of psychotherapy nor can any group clearly demonstrate a consistent superiority in efficacy over all other groups” (p. 5), the following eight broad therapeutic models capture the essence of what is generally accepted in psychotherapeutic circles globally. The psychotherapeutic approach as practiced at Weskoppies and Dr. George Mukhari Hospitals include an understanding of the principles, assumptions, and techniques of the following eight approaches:
The Psychodynamic Approach.
Behaviour, Cognitive, and Cognitive Behavioral Approaches.
Person-Centered Approach.
Existential Approaches.
Gestalt Therapy Approach.
Group Therapy Approaches.
The Ecosystemic Approach.
Integrative Therapy.
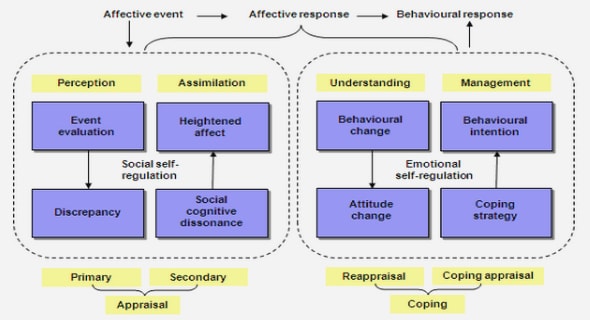
All theories of psychotherapy emphasise one or more of the constructs illustrated in Figure 4.1 below. Figure 4.1 is an illustration of how some commonly used concepts and constructs may be interrelated. Naturally, like any schematic representation, this illustration is only an approximation of the true psychological situation.
All the divergent theories, and conceptual approaches, offer guidelines to psychotherapists to decide what to observe and hence what to do with the observations. In general terms there are two opposing points of view about how to decide what to observe in nature. Albert Einstein for example has stated that firstly we need to create a theory in order to decide which facts to observe, while Sherlock Holmes was convinced that we first need to see the facts before we can create a theory (Messer & Wachtel, 1992). Both points of view are valid in attempting to make sense out of human nature and human behavior, especially when we realise that our thoughts, feelings, beliefs, attitudes, values, motives, and actions inextricably influence each other. In essence, our attitudes and our actions are what will make the difference in how we relate to ourselves and to the people in our environment.
It is not my intention, nor is it possible to summarise all aspects of the following therapeutic approaches. My aim is to highlight only some key features of the therapeutic approaches with relevance to how it is applied within the Weskoppies Hospital culture-sharing therapeutic community. In any multidisciplinary context an integration of the intrapsychic (body and mind), and the interpsychic (interpersonal and intercultural) aspects, of the patient’s functioning needs to be understood, when deciding upon the patient’s rehabilitation process (refer to Chapter 1 Section 1.2.10).
The Psychodynamic Approach
I remember when I first read Freud’s (1976) work on dreams, how fascinated I was by how complex and unpredictable the mind could be. The language of symbols and the power of the unconscious mind, motivated me to record my dreams on a daily basis for several years, many of which I discussed with my therapist, as I was undergoing learning therapy (leerterapie) during my BA Honours years.
I would like to introduce the psychodynamic approach by quoting what Sigmund Freud (1856-1939), the founder of psychoanalysis, once said in private correspondence in 1928, eleven years before his death: “Why was it that none of the pious ever discovered psychoanalysis? Why did it have to wait for a completely Godless Jew?” (Stafford-Clark, 1973, p. 14). In this one short statement, Freud’s verbal behaviour reflects his beliefs, attitude, thoughts, feelings, and motivation, towards God, spirituality, piety, Judaism, and psychotherapy. Freud’s personal life was apparently relatively uneventful, but his ideas have shaped the intellectual climate of many disciplines in the past century.
The psychodynamic approach refers to Freud’s (1976, 1979) psychoanalytical treatment methods based on his psychoanalytic theory, as well as the work carried out by his followers, such as Jung (1963), Klein (1946), Sullivan (1953) and many others. The psychodynamic approach emphasises mainly the intrapsychic (intrapersonal) aspects of an individual’s functioning. When inspecting Figure 4. 1 above (p. 66), the psychodynamic approach would deal with all aspects of a person’s functioning namely, beliefs, attitudes, cognitions, emotions, volition, and the symptoms manifesting in the observable behavior.
In the Weskoppies setting, by focusing on how the patient is repeating his early childhood in his present relationships, I am able to see how he brings his past relationships with significant others, particularly his father, into the session with me. When it becomes relevant I focus on his feelings towards me, because working with the phenomenon of transference is one way of attaining insight. I am also interested in the patient’s dreams, any resistance that he shows, and any other clues triggered by his unconscious processes, which I assume may have a bearing on his present functioning. Allow me to share a portion of my feedback given to an intern after one of my recent live supervision sessions:
“I would like to emphasise one important aspect of the psychotherapeutic relationship of trust, namely the occurrence of transference. Corsini and Wedding, (1995, 2005) have described transference as the emotional bond that develops between the client and the therapist, or between the client and other significant patients. Another description of transference which I came across recently, is given by James Hillman (in Bader & Pearson, 2006a) who defines transference as ‘…that which arrives to replace a real relationship’ (p. 2).
“I would like to focus on the nature of the phenomena that arrives which replaces a real relationship. As frequently observed in our ward rounds the patient shows his disappointment when her/his high (often unrealistic) expectations are not met. The disappointment may have to do with circumstances surrounding the therapist’s skills, the patient’s expectations, the treatment process, or the discharge procedure. The disappointment becomes the focus of discussion during the ward round, or during the therapeutic session at that stage of his treatment, and if the patient is not allowed to speak about his anger, frustration, and helplessness surrounding his disappointment, or if the therapists involved are not equipped to deal with the situation then a stalemate occurs. Consequently the rehabilitation process becomes stuck, leading to the immobilization of growth and hope in the patient.
“What normally happens at this stage of the stalemate, is that the therapist (or mental health worker) takes the easy way out and uses her/his power and authority, by attaching a label to the patient, and influencing the other staff members that the patient is either relapsing, negative, oppositional, aggressive, showing no insight, or manipulative. At this stage, something has arrived to replace a real relationship. The something that has arrived in the relationship which has replaced the real relationship may be referred to as transference, (on the patient’s part) counter-transference (on the therapist’s part) and/or projective identification (again on the patient’s part). We generally regard transference as the impact that the other person’s communication has on us as therapists, while counter-transference may be seen as our ability or inability to understand, absorb, and respond effectively and appropriately to the other person’s communication.
“Transference and counter-transference can be either positive or negative. For many patients, transference may be embedded in another unconscious process known as projective identification, a concept coined by Melanie Klein (Klein, 1946), and discussed by many others such as Waska (1999), of which the therapist may be aware or unaware of. For staff members however, who are not adequately trained to recognize these unconscious processes, their counter-transference (positive or negative), which they communicate unconsciously, may take on the form of power tactics. On the other hand, clinical psychologists while under their internship supervision, undergo transference experientially. Clinical psychologists have been trained to ask questions about the reciprocal impact in the interaction between therapist and client during their psychotherapy supervision training, which is not generally the case with other health professionals. Therefore closely related to transference is the phenomenon of projection and projective identification. The following summary given by Anyara-Essays, (2004) neatly sums up the situation of projection.
“The term ‘projection’ according to Carl G. Jung designates ‘… quite correctly the illusion and unconscious assumption by which I ascribe to my fellow man what largely belongs to myself. I lodge it in him, so to speak’” (p. 1).
“Projective identification is thus a psychological process that can happen between any two persons, especially when one of the two partners has a deep inner need to get rid of some of her or his own parts. When such a person finds a good projection target he or she dumps all those unwanted parts onto (actually into) the other person. Projected qualities are not always negative, even our good qualities may get buried deep within and then projected out (into the therapist) without our conscious knowledge.”
The psychoanalytic approach to the understanding and treatment of mental illnesses has been the most commonly used approach since the start of Weskoppies Hospital; even the street names signify the initial Freudian influence (refer to Chapter 5, Section 5.8). The psychodynamic influence is particularly evident in the psychometric testing and evaluation of observation cases in Ward 23 which will be referred to in Chapter 8 of this thesis.
Getting back to Freud’s comment at the beginning of this section, I am not sure how Freud ever responded to his statement about being a Godless Jew discovering psychoanalysis, or how his friends, family members, or colleagues responded. It is however self-evident that Freud asked many other questions about himself and his theory of psychoanalysis. One can only speculate how pleased or displeased he would be to see how psychotherapy has developed over the past 100 years.
Behaviour, Cognitive, and Cognitive Behavioural Approaches
Initially I was not impressed with behaviour therapy. I found it to be too ordinary, simplistic, and mechanical. I however soon overcame my arrogance towards behaviour therapy when I realized the effectiveness of how relaxation exercises, autogenic training, and self-monitoring tasks reduced and even eradicated negative symptoms. I was particularly influenced by the practical and clear guidelines outlined in the behaviour therapy text book by Walen, Hauserman, and Lavin, (1977).
Burrhus Frederic Skinner (1904-1990), is not a typical behaviour psychotherapist, but rather a renowned researcher in behaviourism. I just happen to enjoy the topics that he addresses in his writings from a behaviourist’s point of view. Issues such as freedom, dignity, values, culture, and the question, ‘What is man?’ may equally belong to the school of phenomenology and existentialism. In his last book Skinner (1976) asserts that: “We have used the instruments of science; we have counted and measured and compared; but something essential to scientific practice is missing in almost in all current discussions of human behavior. It has to do with our treatment of the causes of behavior” (p. 13). In contrast to this statement behavior therapy is not really interested in the cause of mental disorders, but rather in how to remedy the problem.
The philosophical roots of behaviour therapy can be found in the school of behaviourism, which states that psychological matters can be studied scientifically by observing overt behavior, without discussing internal mental states (Rimm & Masters, 1979; Yates, 1970). The behavioural model thus focuses only on observable behaviour. The cognitive behavioural model, as developed by Beck (1976, 1995) however, also addresses intra and interpersonal issues of our psychological functioning. When inspecting Figure 4. 1 (on page 66, the behavioural approach would focus mainly on the observable behavior, while the cognitive behavioural approach would focus mainly on the beliefs, cognitions, emotions, and observable behaviour aspects of the person’s functioning.
It is generally agreed that theories of psychotherapy can be evaluated, discussed, and criticised on three levels, namely, as a sound theory, as useful guidelines for treatment, and as conducive for research. Behaviour, cognitive, and cognitive behavioural therapies have been subjected to, and have had the most published research carried out on them on each of the three levels.
Progressive relaxation, autogenic training, systematic desensitization, role playing, assertion training, hypnotherapy, guided imagery, cognitive restructuring, flooding, implosion, symptom monitoring, assigning tasks and homework are accepted and commonly used techniques in behaviour, cognitive, and cognitive behavioral therapies (Corey, 2005; Prochaska & Norcross, 2007; Walen et al., 1977; Wolberg, 1977).
In behaviour therapy as implemented at Weskoppies Hospital, a thorough assessment of the patient’s current observable behaviour is conducted. Sometimes the patient is asked to monitor his activities so that baseline data can be created in order to evaluate any visible changes. In collaboration with the patient concrete goals are created. New coping skills are constantly taught in the therapy sessions, often through role playing and the patient is encouraged to use the skills in his everyday situations.
In cognitive behaviour therapy the focus is on how the patient’s internal dialogue and thinking processes influences his behaviour. An active and directive therapeutic style is used. Therapy sessions are present-centered, time limited, and structured. The patient’s self-defeating and self-handicapping beliefs are explored, inquired into, and challenged. This is done as follows: The patient is encouraged in collaboration with the therapist (the therapeutic alliance) to work out how his cognitive triad of negative automatic thoughts (NAT’s) are attached to his beliefs (intermediate and core beliefs). Techniques used may include role playing, modelling, coaching, assertion training, completing homework assignments, and relaxation methods. (Beck, 1995; Corey, 2005; Hollon & Beck, 1994).
Regarding transference reactions (that which arrives to replace a real relationship), in the context of common therapeutic processes found in diverse approaches, Beck (in Marmor, 1987), explains that by pinpointing the thought preceding the feeling expressed by the patient which triggers the transference reaction, can rapidly get at the material that is relevant to the transference reaction in a much shorter time than by questioning and probing. Beck’s daughter Judith Beck (Commitment, 2007) explains how thoughts precede emotions: “Individuals interpret situations in various ways and react emotionally in accordance with that interpretation. For example your friend is late. If you think, ’She must not care about me,’ your emotional reaction is likely to be one of sadness. If you think, ‘What if something terrible happened to her?’ you are likely to feel anxious. If you think, ‘How dare she keep me waiting!’ you will probably feel angry. Your perceptions, in the form of your thoughts, influence your emotional reactions” (pp.4-5). Beck (in Zeig 1987) clarifies the importance of the therapist’s awareness of his/her own feelings and thought patterns which influences therapy outcome. “So that’s the second point I want to make about transference. I certainly believe one should be aware of it as much as possible. It plays an important role in understanding the patient. There is another thing we should keep in mind about transference reactions. …If you’re not aware of the way the patient reacts toward you, the whole therapy can become counterproductive” (p. 276). It is reassuring to note that when the understanding of a psychoanalytical term like transference is truly grasped, then it can be observed in any interpersonal interaction, as clearly illustrated in the above quote by Beck (in Zeig 1987).
The concept of behaviour modification traditionally belongs to behaviour therapy. In the Weskoppies Hospital setting the concept of behaviour modification has very often been used as an excuse for punishment. Behaviour modification as understood by clinical psychologists, explained and taught by psychiatrists, and implemented by nurses, especially by the night staff, and weekend staff, has led to much debate and confusion, and has been counter therapeutic to patients. This confusion seems to be the projections that health workers place on their understanding of the concept of behavior modification. Based on the idea of reward and punishment the emphasis rather is supposed to fall on reinforcement and extinction. The principles of the token economy system worked for a while at Westfort hospital in the early 1990’s (referred to in Chapter 6 Section 6.3). Currently in the Weskoppies setting, behaviour modification has become a matter of arbitrary assigning and withdrawing privileges, which has different implications in reality. For example patients are:
kept in their pyjamas;
not allowed to visit the tuck-shop;
not allowed to attend occupational therapy;
not allowed to attend group therapy;
kept in seclusion;
transferred to closed ward for at least three months.
In the hospital system wrong, dysfunctional, unrealistic, and faulty behaviours are often reinforced. For example the patient’s dagga use, assertive behaviour, and compliance has often led to contradictory and paradoxical ways of understanding such behaviours on the part of patient and staff alike. Misunderstandings and confusion arises, which detracts from a real relationship, resulting in the very strong likelihood of projection, transference, and counter- transference to take place.
CONTENTS
Acknowledgements
Summary
Declaration
List of Tables
List of Figures
Chapter One: Multicultural Dimensions of Psychological Treatment
1.1 Introduction
1.2 Multicultural Dimensions or Influences that Play a Part in the Psychiatric Hospital
1.3 The Health Care Professional as a Therapeutic Person
1.4 Psychotherapy
1.5 Ethnographic Research
1.6 Motivation
1.7 Objectives and Aims
1.8 Presentation
Chapter Two: Methodology
2.1 Introduction
2.2 Quantitative Research
2.3 Qualitative Research
2.4 Ethnographic Research
2.5 Method of the Present Study
2.6 Conclusion
Chapter Three: Psychotherapy
3.1 Introduction
3.2 Definition of Psychotherapy
3.3 Mechanisms and Ingredients of Psychotherapy
3.4 Research and Clinical Evidence
3.5 International Psychotherapy
3.6 Eurocentric Psychotherapy
3.7 African Psychotherapy
3.8 Ecosystemic Psychotherapy
3.9 Group Psychotherapy
3.10 Conclusion
Chapter Four: Initiating Students into the Culture of Therapeutic Psychology
4.1 Theoretical Perspectives in Psychotherapy
4.2 The Psychodynamic Approach
4.3 Behaviour, Cognitive, and Cognitive Behavioural Approaches
4.4 Person-Centered Approach
4.5 Existential Approaches
4.6 The Gestalt Therapy Approach
4.7 Group Therapy Approaches
4.8 Ecosystemic Psychotherapy
4.9 Integrative Psychotherapy
4.10 The Psychotherapist as a Role Model
4.11 The Psychologist as Therapist and Scientist
4.12 Research and Psychotherapy
4.13 Theoretical Perspectives in Training and Supervision
4.14 In Vivo (Live) Supervision
4.15 Towards an Effective Multicultural Therapeutic Community
4.16 Conclusion
Chapter Five: Professional Culture-Sharing the Hospital
5.1 Daily Hand-Over Meetings
5.2 Ward 59 Culture-Sharing Group
5.3 A Day in the Life of a Ward Round
5.4 Male State Patients
5.5 Compliance to Medication
5.6 Family Support
5.7 Dagga Use and Abuse
5.8 The Hospital Setting
5.9 A Therapeutic Community
5.10 How The New Mental Health Care Act is Conducive to a Therapeutic Community
5.11 Restraining Factors which Delay Patient’s Discharge
5.12 Rehabilitation Programmes: Translating Words into Action
5.13 Conclusion
Chapter Six: Professional Culture-Sharing in Ward 59: An Open Ward
6.1 Introduction
6.2 The Ecosystemic Approach in Action: A Therapeutic Community in the Making
6.3 Westfort Hospital
6.4 Accommodating the Others’ Spirituality
6.5 How “Acting Out” Rituals Compliments Treatment
6.6 An Example of “Prescribing the Symptom”
6.7 Open and Closed Wards
6.8 Rehabilitation Programmes
6.9 A Family Day in Ward 59
6.10 Psychotherapeutic Approaches Used in the Open Ward
6.11 Practical Issues in Training and Supervision
6.12 Towards an Effective Multicultural Therapeutic Community
6.13 Conclusion
Chapter Seven: Professional Culture-Sharing Group in Wards 65 and 66
7.1 Introduction
7.2 Wards 65 and 66 (Semi-Closed and Semi-Open Wards)
7.3 Group Therapy
7.4 A Therapeutic Music Group
7.5 Psychotherapeutic Approaches in the Semi-Open and Semi-Closed Wards
7.6 Practical Issues in Training and Supervision
7.7 Towards an Effective Multicultural Therapeutic Community
7.8 Conclusion
Chapter Eight: Professional Culture-Sharing in Wards 22 and 23
8.1 Introduction
8.2 Ward 22 Rehabilitation Maximum Security Ward
8.3 Ward 23 Observation Maximum Security Ward
8.4 Practical Issues in Training and Supervision
8.5 Towards an Effective Multicultural Therapeutic Community
8.6 Conclusion
Chapter Nine: Understanding the Patient in Context
9.1 Introduction
9.2 Meta-Influences Inhibiting a Multicultural Therapeutic Community
9.3 Understanding the Patient
9.4 Towards an Effective Multicultural Therapeutic Community
9.5 Conclusion
Chapter Ten: Conclusions and Implications
10.1 Introduction
10.2 Recommendations and Ethical Considerations
10.3 Ethical Considerations Relating to the Present Study
10.4 Future Research
10.5 Conclusion
References
GET THE COMPLETE PROJECT